Traumatic brain injury: molecule from Kiel supports brain repair
International research team has discovered how repair after a brain injury can be improved by influencing immune cells
With a traumatic brain injury, a varying number of nerve cells in the brain die off, depending on the severity of the injury. Such brain injuries can impair someone’s concentration, the ability to make decisions, learning and memory. A molecule developed by Professor Stefan Rose-John, member of the Cluster of Excellence "Precision Medicine in Chronic Inflammation" (PMI), and Executive Director of the Institute of Biochemistry at Kiel University (CAU), could trigger a mechanism that repairs this damage, as indicated by new research results which Rose-John and international researchers under the leadership of the University of Queensland in Brisbane, Australia recently published in the prestigious scientific journal Cell.
The researchers investigated how the immune system in the brains of mice interacts with brain nerve cells after an injury, and how this influences the memory and the ability to learn. "Previously, we assumed that after a brain injury, specific immune cells in the brain, the microglia, promote inflammation of the brain and thereby lead to a reduction in cognitive skills," reported the lead author of the publication, Dr. Jana Vukovic, from the University of Queensland. "However, when we removed microglia from mice we were surprised that there was absolutely no change in their behaviour or ability to repair brain tissue," continued Vukovic. In response to this finding, the research team then stimulated increased formation of new microglia in animal experiments and discovered that this promotes the repair of nerve cells. "The rejunevated microglia improved the mice's learning an memory, preserved tissue loss and stimulated the birth of neurons," said Vukovic.
Interleukin-6 promotes repair
The driving force behind this regenerative process is the signaling molecule Interleukin-6 (IL-6): when the researchers blocked it completely in experiments, the regenerative effect of microglia also disappeared. When they increased the amount of IL-6 present, they stimulated the process. The signaling molecule is an important chemical messenger which raises the alarm if inflammatory reactions occur, for example, when it is secreted in increased quantities, and thus regulates immune responses. It can function via two different signaling pathways: in the "traditional" signaling pathway, IL-6 specifically binds to a receptor which is only present in certain cells, such as liver cells. Together, they then bind to another receptor subunit on the same cell, the so-called gp130 protein, thereby triggering a reaction in the cell. In the alternative so-called "IL-6 trans-signaling pathway", on the other hand, IL-6 can affect every cell in the body under certain circumstances. The specific IL-6 receptor is also present in soluble form in the blood. IL-6 can bind to these free receptors circulating in the bloodstream. This compound then binds to a gp130-receptor, which is present on all cells, and triggers a reaction in the cell.
A designer molecule as a molecular diagnostic tool
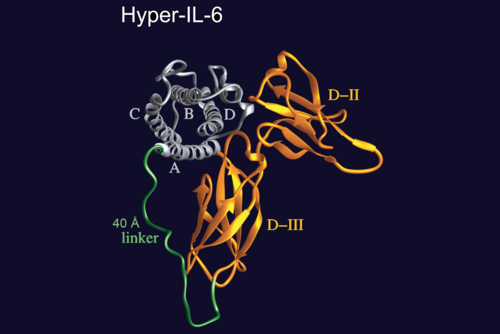
Rose-John discovered this trans-signaling pathway, which is involved in many physiological processes, and has achieved pioneering research in investigating its central importance. "We have developed several molecular tools over the past few years that we can use to test which signaling pathway is active in a particular disease pattern," explained Rose-John. These molecular tools include the artificial molecule "Hyper-IL-6", which was also used in the current study. It consists of the signaling molecule Interleukin 6 (IL-6) and its specific receptor in soluble form, i.e. not bound with a cell. Together, they form a completely new molecule which does not exist in this form in nature. Just like its naturally-occurring individual components, this new molecule also stimulates the IL-6 trans-signaling pathway, but it is significantly more effective since IL-6 and its receptor no longer have to "find each other" in the blood, like they would normally do in nature.
Regeneration via the IL-6 trans-signaling pathway
In the current study, Hyper-IL-6 showed a positive effect: after administering the molecule to injured nerve cells, more microglia formed, which in turn led to the formation of new nerve cells, and ultimately to an improvement of the symptoms. "The results show that the newly-discovered regenerative effect of microglia after a brain injury is triggered by IL-6 via the trans-signaling pathway," said Rose-John. "This observation is also interesting, because up until now we had no idea how IL-6 works in the brain."
In future, the results could enable the development of new drugs to alleviate learning and memory deficits after the nerve cells have been damaged. They therefore offer promising potential for treating a variety of neurological disorders such as brain injury, dementia and other neurodegenerative diseases.
Original publication:
Emily F. Willis, …Stefan Rose-John, Marc J. Ruitenberg, and Jana Vukovic: Repopulating Microglia Promote Brain Repair in an IL-6-Dependent Manner, Cell (2020).
DOI: 10.1016/j.cell.2020.02.013
Further information:
Institute of Biochemistry, Kiel University
Collaborative Research Centre (CRC) 877 "Proteolysis as a Regulatory Event in Pathophysiology"
Vukovic Group - Neuroimmunology and Cognition, The University of Queensland, Australia
With the designer molecule "Hyper-IL-6", an IL-6 molecule is firmly bound to its specific soluble receptor. The new molecule can thus activate the IL-6 trans-signaling pathway much more effectively than both molecules independently.
Professor Stefan Rose-John, member of the Cluster of Excellence "Precision Medicine in Chronic Inflammation", former Executive Director of the Institute of Biochemistry at Kiel University (CAU), and head of the Collaborative Research Centre (CRC) 877 "Proteolysis as a Regulatory Event in Pathophysiology".
About the Cluster of Excellence PMI
The Cluster of Excellence "Precision Medicine in Chronic Inflammation" (PMI) is being funded from 2019 to 2025 through the German Excellence Strategy (ExStra). It succeeds the "Inflammation at Interfaces” Cluster, which was already funded in two periods of the Excellence Initiative (2007-2018). Around 300 members from eight institutions at four locations are involved: Kiel (Kiel University, University Medical Center Schleswig-Holstein (UKSH), Muthesius University of Fine Arts and Design, Kiel Institute for the World Economy (IfW), Leibniz Institute for Science and Mathematics Education (IPN)), Lübeck (University of Lübeck, University Medical Center Schleswig-Holstein (UKSH)), Plön (Max Planck Institute for Evolutionary Biology) and Borstel (Research Center Borstel - Leibniz Lung Center).
The goal is to translate interdisciplinary research findings on chronic inflammatory diseases of barrier organs to healthcare more intensively, as well as to fulfil previously unsatisfied needs of the patients. Three points are important in the context of successful treatment, and are therefore at the heart of PMI research: the early detection of chronic inflammatory diseases, the prediction of disease progression and complications, and the prediction of individual responses to treatment.
Press office
fbuhse@uv.uni-kiel.de+49 (0)431/880 4682 https://precisionmedicine.de
Cluster of Excellence "Precision Medicine in Chronic Inflammation"
Scientific Office
Head: Dr. habil. Susanne Holstein Postal
Christian-Albrechts-Platz 4, 24118 Kiel, Germany
Contact: Sonja Petermann
+49 (0)431 880-4850, fax: +49 (0)431 880-4894
spetermann@uv.uni-kiel.de
Twitter: PMI @medinflame